Volume 18, Issue 2 (7-2021)
J Res Dev Nurs Midw 2021, 18(2): 36-40 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Afolalu O O, Atekoja O E, Akingbade O, Jolayemi K I, Oyewumi Z O, Oyelabi B D et al . Knowledge and Perceived Effect of Polypharmacy and Potentially Inappropriate Medication Use among Nurses in a Nigerian Tertiary Hospital. J Res Dev Nurs Midw 2021; 18 (2) :36-40
URL: http://nmj.goums.ac.ir/article-1-1318-en.html
URL: http://nmj.goums.ac.ir/article-1-1318-en.html
Olamide Olajumoke Afolalu1 

 , Oluwabusolami Esther Atekoja2
, Oluwabusolami Esther Atekoja2 

 , Oluwadamilare Akingbade3
, Oluwadamilare Akingbade3 

 , Karimat Itunu Jolayemi4
, Karimat Itunu Jolayemi4 

 , Zaccheus Opeyemi Oyewumi5
, Zaccheus Opeyemi Oyewumi5 

 , Boluwatife Deborah Oyelabi6
, Boluwatife Deborah Oyelabi6 

 , Semiu Opeyemi Adeyeye7
, Semiu Opeyemi Adeyeye7 




 , Oluwabusolami Esther Atekoja2
, Oluwabusolami Esther Atekoja2 

 , Oluwadamilare Akingbade3
, Oluwadamilare Akingbade3 

 , Karimat Itunu Jolayemi4
, Karimat Itunu Jolayemi4 

 , Zaccheus Opeyemi Oyewumi5
, Zaccheus Opeyemi Oyewumi5 

 , Boluwatife Deborah Oyelabi6
, Boluwatife Deborah Oyelabi6 

 , Semiu Opeyemi Adeyeye7
, Semiu Opeyemi Adeyeye7 


1- Department of Nursing Science, Osun State University, Nigeria , olamide.afolalu@uniosun.edu.ng
2- Department of Nursing Science, Olabisi Onabanjo University, Ogun State, Nigeria
3- The Nethersole School of Nursing, Chinese University of Hong Kong, China
4- Department of Nursing Science, Adeleke University, Osun State, Nigeria
5- Department of Nursing Science, Achievers University, Ondo State, Nigeria
6- Department of Nursing Science, Osun State University Osogbo, Osun State, Nigeria
7- Department of Nursing Science, Ladoke Akintola University of Technology, Ogbomoso, Oyo State, Nigeria
2- Department of Nursing Science, Olabisi Onabanjo University, Ogun State, Nigeria
3- The Nethersole School of Nursing, Chinese University of Hong Kong, China
4- Department of Nursing Science, Adeleke University, Osun State, Nigeria
5- Department of Nursing Science, Achievers University, Ondo State, Nigeria
6- Department of Nursing Science, Osun State University Osogbo, Osun State, Nigeria
7- Department of Nursing Science, Ladoke Akintola University of Technology, Ogbomoso, Oyo State, Nigeria
Keywords: Polypharmacy [MESH], Potentially inappropriate medication list [MESH], knowledge [MESH], perception [MESH].
Full-Text [PDF 869 kb]
(1161 Downloads)
| Abstract (HTML) (3455 Views)




Full-Text: (1471 Views)
Highlights:
What is current knowledge?
Polypharmacy and use of inappropriate medication are issues increasingly affecting the health care system. Despite nurses’ engagement and useful role in prevention of drug-related issues, the awareness regarding consequences arising from polypharmacy and also the use of inappropriate medication is considerably low.
What is new here?
Assessment of knowledge and perception of polypharmacy effects and inappropriate medication use among nurses fosters identification of patients at increased risk of polypharmacy. It also promotes anticipation of potential complications that could arise from multiple drugs and medications used inappropriately.
Introduction
Polypharmacy (PP) and inappropriate medication use (IMU) are ubiquitous problems that rapidly invade the healthcare system, with direct and indirect impact on nursing care. Sometimes, patients take a complex combination of drugs and supplements, but this can cause more harm than good. It is estimated that more than half of all medications are prescribed, distributed, or traded inappropriately, with many of these leading to preventable harm (1).
According to Masnoon et al, PP is a patient safety issue mostly concerned with situations where patients take five or more medications simultaneously (2). The global prevalence of PP has increased tremendously in the last 20 years with variations across countries ranging between 7% and 90% in different populations (3, 4). In the United States, the prevalence of PP has been estimated to be 10% among the general population and 30% among the older adults (5). A similarly high prevalence has been reported in some African countries such as Uganda, Togo, and Nigeria (6–8).
More recently, research indicated that PP is associated with drug reactions and acute care hospitalization in four out of every one thousand people annually. It is also associated with annual costs estimated at $180 billion in the US alone (5).
Studies have shown that PP is the main risk for potentially inappropriate medication prescription (9,10). Nurses have an important role in the management of PP- and PIM-associated consequences. They are principally involved in the care process from admission to discharge. Deprescribing is a public phenomenon involving planned and supervised method of dose reduction or termination of medication, which may be harmful to the user (11). Previous studies demonstrated the inadequate knowledge of clinicians and resources to evaluate care and embrace deprescribing in patients experiencing multiple comorbidities and PP (12–14).
Various reasons for Nurses’ lack of confidence in addressing polypharmacy were reported, additionally to issues of withdrawal, ability to observe, discontinue or modify a medicine prescribed by another care giver, lack of clarity related to tapering, failure in disorder management, and different harmful effects (13). Despite the need for raising awareness in order to deal with PP and medication management within primary care, the implementation of evidence-based solutions has been sub-optimal (12,14,15).
Several studies have shown an increasing prevalence of PP and IMU in the management of multi-morbidity, especially in the elderly. Some studies also recognized the need for educational training of nurses about medication prescription as a potential strategy to minimize IMU (16). However, very little is known about the knowledge of nurses on the effects of PP and IMU. Given that the safe administration of medication is an important role of nurses, adequate knowledge of nurses is essential to prevent adverse health outcomes that could arise from PP and IMU (17). This study aimed to provide an overview of the current state of nurses' knowledge and perception about PP and IMU. The guiding objectives of the study are : (a) to investigate nurses’ knowledge and perception of PP and IMU, (b) to identify the causes of PP and IMU, (c) to assess their perceived effect of PP and IMU, and (d) to identify the perceived factors preventing IMU and PP.
Methods
Study design and setting
This descriptive, cross-sectional study was carried out in November 2020 to elicit knowledge and perception of nurses in Ladoke Akintola University of Technology (LAUTECH) Teaching Hospital Osogbo (Osun State, Nigeria) about PP and IMU. The hospital offers tertiary care services and serves as a referral center to neighboring health institutions within the Oyo and Osun States. It has 32 wards and over 10 clinical nurse specialty areas (mental, orthopedics, perioperative nursing, nurse anesthetists, ophthalmology, accident and emergency, nephrology, pediatric, and oncology nursing).
The inclusion criterion was being a nurse in the hospital for not less than a year. The researchers assumed that experience on PP could only be gained via work experience. Nurse mangers were excluded because they are less likely to have direct interaction with patients.
Sample size calculation
A list of nurses working in various units/wards of the hospital was obtained from the hospital’s administrative department. From a total population of 300 nurses, sample size was determined as 171 using the Taro Yamane formula, at 95% confidence level. After adjusting sample size for 10% non-response rate, a sample size of 190 was considered for the study. The subjects were selected via computer-generated random sampling to eliminate bias. Stratification was further applied to ensure adequate representation of nurses across various specialty areas within the hospital.
Data collection instrument
A researcher-made questionnaire was developed after an extensive review of the literature. The questionnaire were scored based on a Likert type scale and consisted of 35 questions comprising five sections:
Section A: demographic factors
Section B: Nurses' knowledge and perception of PP and IMU
Section C: the causes of PP and IMU
Section D: effects of PP and IMU
Section E: factors preventing PP and IMU.
Validity and reliability of the instrument
The content and face validity of the questionnaire were ascertained by the research team (two clinical and research nurses as well as four public health nurse specialists). Data from content validity showed that all 35 items had high index of content validity (I-CVI) of 0.75 in all domains. Next, a pilot study was carried out to determine the instrument’s reliability by administering 10% (19) of the questionnaires to nurses in another setting (the State Specialist Hospital in Oshogbo). A test-retest reliability method was administered at an interval of two weeks to determine the reproducibility of the questionnaire (18). Consequently, a Cronbach's alpha score of 0.77 was obtained, indicating the validity of and reliability of the instrument (19).
Data collection
Ethical approval was obtained from the ethical and research committees of the LAUTECH Teaching Hospital with the code of ethics (LTH/EC/2020/11/482). Written informed consent was also taken from the participants. Given that the study was carried out during the COVID-19 pandemic, strict precautionary measures were taken to minimize risk of coronavirus transmission. Careful consideration was given to ensure that subjects were not sampled twice. The participants were encouraged to complete the questionnaire independently to minimize sharing views and information between the subjects. Overall, 190 questionnaires were distributed and fully answered. Two members of the research team (OA and BO) were present throughout data collection to provide clarifications. Confidentiality and anonymity of personal information were maintained throughout the study.
Data analysis
Data were analyzed using the statistical package for social sciences (SPSS) version 25.0. Descriptive statistics including mean, frequencies, percentages, and standard deviation were used to describe data. Association between categorical and continuous variables was investigated using the chi-square and Pearson correlation coefficient at statistical significance of 0.05.
Results
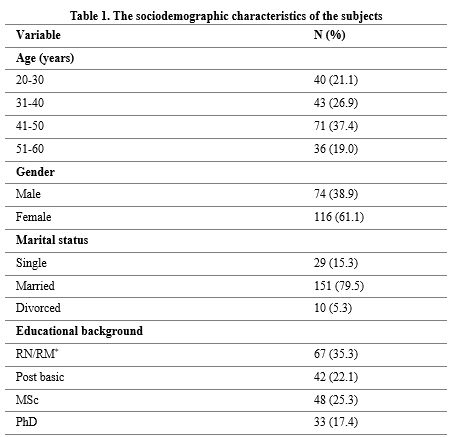
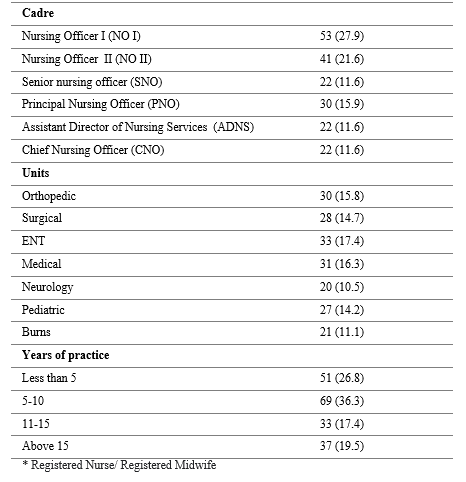
Sociodemographic characteristics of the subjects
The sociodemographic data of the subjects are shown in table 1
Knowledge and perception of PP and IMU among nurses
The result showed that 90% of the respondents have heard of PP and 87.4% agreed that PP is the use of different drugs for the treatment of a single disease. Likewise, 93.2% agreed that inappropriate medication should be entirely avoided, while 64.2% claimed that PP can lead to IMU. The assessment of respondents’ level of knowledge of PP and IMU was done by assigning a score value of "1" to each correct response and a score of "0" to incorrect responses to make a total score of 5. Interquartile percent (25%, 50%, and 75%) was used to grade knowledge into poor, average, and good. Findings of the study revealed that 11 subjects (5.8%) had poor knowledge of PP, 19 (10%) had average knowledge, and 160 (84.2%) had good knowledge of PP and IMU.
Perceived causes of PP and IMU
Data on perceived causes of PP and IMU revealed that 58.9% of the subjects expressed that presence of co-existing conditions and chronic diseases as reasons for PP, while 65.3% believed that visiting multiple physicians for medical problems is the source of PP. In addition, 53.1% of the subjects disagreed with inadequate documentation, while 64.3% of the subjects believed that obtaining information from families and the internet contribute to PP and IMU. Furthermore, 52.1% of the respondents agreed that increasing age is a predisposing factor to IMU. However, the rest of the respondents (57.8%) claimed that poor communication between patients and caregivers could be a possible cause of PP. Moreover, 70.5% of the subjects believed that easy access to different medications is a major causative factor.
What is current knowledge?
Polypharmacy and use of inappropriate medication are issues increasingly affecting the health care system. Despite nurses’ engagement and useful role in prevention of drug-related issues, the awareness regarding consequences arising from polypharmacy and also the use of inappropriate medication is considerably low.
What is new here?
Assessment of knowledge and perception of polypharmacy effects and inappropriate medication use among nurses fosters identification of patients at increased risk of polypharmacy. It also promotes anticipation of potential complications that could arise from multiple drugs and medications used inappropriately.
Introduction
Polypharmacy (PP) and inappropriate medication use (IMU) are ubiquitous problems that rapidly invade the healthcare system, with direct and indirect impact on nursing care. Sometimes, patients take a complex combination of drugs and supplements, but this can cause more harm than good. It is estimated that more than half of all medications are prescribed, distributed, or traded inappropriately, with many of these leading to preventable harm (1).
According to Masnoon et al, PP is a patient safety issue mostly concerned with situations where patients take five or more medications simultaneously (2). The global prevalence of PP has increased tremendously in the last 20 years with variations across countries ranging between 7% and 90% in different populations (3, 4). In the United States, the prevalence of PP has been estimated to be 10% among the general population and 30% among the older adults (5). A similarly high prevalence has been reported in some African countries such as Uganda, Togo, and Nigeria (6–8).
More recently, research indicated that PP is associated with drug reactions and acute care hospitalization in four out of every one thousand people annually. It is also associated with annual costs estimated at $180 billion in the US alone (5).
Studies have shown that PP is the main risk for potentially inappropriate medication prescription (9,10). Nurses have an important role in the management of PP- and PIM-associated consequences. They are principally involved in the care process from admission to discharge. Deprescribing is a public phenomenon involving planned and supervised method of dose reduction or termination of medication, which may be harmful to the user (11). Previous studies demonstrated the inadequate knowledge of clinicians and resources to evaluate care and embrace deprescribing in patients experiencing multiple comorbidities and PP (12–14).
Various reasons for Nurses’ lack of confidence in addressing polypharmacy were reported, additionally to issues of withdrawal, ability to observe, discontinue or modify a medicine prescribed by another care giver, lack of clarity related to tapering, failure in disorder management, and different harmful effects (13). Despite the need for raising awareness in order to deal with PP and medication management within primary care, the implementation of evidence-based solutions has been sub-optimal (12,14,15).
Several studies have shown an increasing prevalence of PP and IMU in the management of multi-morbidity, especially in the elderly. Some studies also recognized the need for educational training of nurses about medication prescription as a potential strategy to minimize IMU (16). However, very little is known about the knowledge of nurses on the effects of PP and IMU. Given that the safe administration of medication is an important role of nurses, adequate knowledge of nurses is essential to prevent adverse health outcomes that could arise from PP and IMU (17). This study aimed to provide an overview of the current state of nurses' knowledge and perception about PP and IMU. The guiding objectives of the study are : (a) to investigate nurses’ knowledge and perception of PP and IMU, (b) to identify the causes of PP and IMU, (c) to assess their perceived effect of PP and IMU, and (d) to identify the perceived factors preventing IMU and PP.
Methods
Study design and setting
This descriptive, cross-sectional study was carried out in November 2020 to elicit knowledge and perception of nurses in Ladoke Akintola University of Technology (LAUTECH) Teaching Hospital Osogbo (Osun State, Nigeria) about PP and IMU. The hospital offers tertiary care services and serves as a referral center to neighboring health institutions within the Oyo and Osun States. It has 32 wards and over 10 clinical nurse specialty areas (mental, orthopedics, perioperative nursing, nurse anesthetists, ophthalmology, accident and emergency, nephrology, pediatric, and oncology nursing).
The inclusion criterion was being a nurse in the hospital for not less than a year. The researchers assumed that experience on PP could only be gained via work experience. Nurse mangers were excluded because they are less likely to have direct interaction with patients.
Sample size calculation
A list of nurses working in various units/wards of the hospital was obtained from the hospital’s administrative department. From a total population of 300 nurses, sample size was determined as 171 using the Taro Yamane formula, at 95% confidence level. After adjusting sample size for 10% non-response rate, a sample size of 190 was considered for the study. The subjects were selected via computer-generated random sampling to eliminate bias. Stratification was further applied to ensure adequate representation of nurses across various specialty areas within the hospital.
Data collection instrument
A researcher-made questionnaire was developed after an extensive review of the literature. The questionnaire were scored based on a Likert type scale and consisted of 35 questions comprising five sections:
Section A: demographic factors
Section B: Nurses' knowledge and perception of PP and IMU
Section C: the causes of PP and IMU
Section D: effects of PP and IMU
Section E: factors preventing PP and IMU.
Validity and reliability of the instrument
The content and face validity of the questionnaire were ascertained by the research team (two clinical and research nurses as well as four public health nurse specialists). Data from content validity showed that all 35 items had high index of content validity (I-CVI) of 0.75 in all domains. Next, a pilot study was carried out to determine the instrument’s reliability by administering 10% (19) of the questionnaires to nurses in another setting (the State Specialist Hospital in Oshogbo). A test-retest reliability method was administered at an interval of two weeks to determine the reproducibility of the questionnaire (18). Consequently, a Cronbach's alpha score of 0.77 was obtained, indicating the validity of and reliability of the instrument (19).
Data collection
Ethical approval was obtained from the ethical and research committees of the LAUTECH Teaching Hospital with the code of ethics (LTH/EC/2020/11/482). Written informed consent was also taken from the participants. Given that the study was carried out during the COVID-19 pandemic, strict precautionary measures were taken to minimize risk of coronavirus transmission. Careful consideration was given to ensure that subjects were not sampled twice. The participants were encouraged to complete the questionnaire independently to minimize sharing views and information between the subjects. Overall, 190 questionnaires were distributed and fully answered. Two members of the research team (OA and BO) were present throughout data collection to provide clarifications. Confidentiality and anonymity of personal information were maintained throughout the study.
Data analysis
Data were analyzed using the statistical package for social sciences (SPSS) version 25.0. Descriptive statistics including mean, frequencies, percentages, and standard deviation were used to describe data. Association between categorical and continuous variables was investigated using the chi-square and Pearson correlation coefficient at statistical significance of 0.05.
Results
Sociodemographic characteristics of the subjects
The sociodemographic data of the subjects are shown in table 1
Knowledge and perception of PP and IMU among nurses
The result showed that 90% of the respondents have heard of PP and 87.4% agreed that PP is the use of different drugs for the treatment of a single disease. Likewise, 93.2% agreed that inappropriate medication should be entirely avoided, while 64.2% claimed that PP can lead to IMU. The assessment of respondents’ level of knowledge of PP and IMU was done by assigning a score value of "1" to each correct response and a score of "0" to incorrect responses to make a total score of 5. Interquartile percent (25%, 50%, and 75%) was used to grade knowledge into poor, average, and good. Findings of the study revealed that 11 subjects (5.8%) had poor knowledge of PP, 19 (10%) had average knowledge, and 160 (84.2%) had good knowledge of PP and IMU.
Perceived causes of PP and IMU
Data on perceived causes of PP and IMU revealed that 58.9% of the subjects expressed that presence of co-existing conditions and chronic diseases as reasons for PP, while 65.3% believed that visiting multiple physicians for medical problems is the source of PP. In addition, 53.1% of the subjects disagreed with inadequate documentation, while 64.3% of the subjects believed that obtaining information from families and the internet contribute to PP and IMU. Furthermore, 52.1% of the respondents agreed that increasing age is a predisposing factor to IMU. However, the rest of the respondents (57.8%) claimed that poor communication between patients and caregivers could be a possible cause of PP. Moreover, 70.5% of the subjects believed that easy access to different medications is a major causative factor.



Perceived effects of PP and IMU
The result of this study showed that 145 subject (76.3%) agreed that one of the perceived effects of PP is increased tendency for medical error, and 146 subjects (76.9%) believed that it increases the risk of drug-drug interactions. Moreover, 85.3% of the subjects expressed that PP causes adverse drug reactions and 49.4% believed that it increases the risk for cognitive impairment. Furthermore, 136 subjects (71.6%) agreed that PP and IMU do not accelerate recovery from illness but will cause antimicrobial resistance (41.1%).
Nurses within the nursing officer (NO 1) cadre had good knowledge of PP compared to those in other nursing cadres (mean rank = 56.75), but this difference was not statistically significant (P=0.20). Also, nurses’ highest level of education attainment significantly influenced their knowledge about PP and IMU (P=0.002). There was no significant association between years of practice and knowledge about PP and IMU (Table 2). Furthermore, there was a positive correlation between the respondents’ age and their knowledge of PP (r = 0.204, Sig = 0.016).
There was a significant negative relationship between level of knowledge about PP and the perceived effect of PP and IMU (r= 0.605, P=0.000) (Table 3).
The result of this study showed that 145 subject (76.3%) agreed that one of the perceived effects of PP is increased tendency for medical error, and 146 subjects (76.9%) believed that it increases the risk of drug-drug interactions. Moreover, 85.3% of the subjects expressed that PP causes adverse drug reactions and 49.4% believed that it increases the risk for cognitive impairment. Furthermore, 136 subjects (71.6%) agreed that PP and IMU do not accelerate recovery from illness but will cause antimicrobial resistance (41.1%).
Nurses within the nursing officer (NO 1) cadre had good knowledge of PP compared to those in other nursing cadres (mean rank = 56.75), but this difference was not statistically significant (P=0.20). Also, nurses’ highest level of education attainment significantly influenced their knowledge about PP and IMU (P=0.002). There was no significant association between years of practice and knowledge about PP and IMU (Table 2). Furthermore, there was a positive correlation between the respondents’ age and their knowledge of PP (r = 0.204, Sig = 0.016).
There was a significant negative relationship between level of knowledge about PP and the perceived effect of PP and IMU (r= 0.605, P=0.000) (Table 3).



Discussion
Nurses are strategically positioned to ensure holistic healthcare services are provided to patients, especially concerning medication administration. In this regard, we assessed the knowledge and perception of nurses about the effects of PP and IMU on patients.
The knowledge level among our respondents was similar to findings of a cross-sectional study conducted in four tertiary care facilities in Nigeria. The study showed that the overall knowledge score was above average as most subjects (84.7%) were confident of their ability to prescribe rationally for elderly patients and to deal perfectly with clinical conditions affecting the cardiovascular, endocrine, and gastrointestinal systems (20).
The results of our study showed that 84.2% had good knowledge of PP and IMU, as 90% of the respondents have heard of PP and 87.4% agreed that PP is the use of different drugs for the treatment of a single disease. The high level of knowledge of nurses in our study can be related to their functional role and proximity to the patients in medication management. The knowledge possessed by nurses allows them to link the patient's symptoms to effects or side effects of the drugs prescribed (21) and to increase therapeutic effects of the prescribed medications.
In our study, 93.2% of the subjects agreed that IMU should be entirely avoided, and 64.2% claimed that PP can lead to IMU. This present study is at variance with the submission of a study that identified numerous reasons for Nurses’ lack of confidence in addressing PP as, considerations for withdrawal, inability to observe, stop or modify a previously prescribed drug, and other detrimental effects (13). Training programs that encourage continuing education of nurses and organization of seminars and workshops for care providers involved in medication management will reduce medication-related adverse outcomes (22).
Based on the results, having many co-existing conditions and chronic diseases is one of the reasons for PP among patients. Moreover, visiting multiple physicians for the same medical problem is another reason for IMU. Our subjects also stated that advancing age may predispose patients to IMU, which is in line with findings of a previous study (23). This could be due to the fact that chronic diseases are often more common among the older population. Patients suffering from comorbidities always require multiple medications to control symptoms. Also, increased availability of different medications might be another major factor that contribute to PP and IMU. This factor may have resulted in modification in the pattern of prescription, with the advent of a new specific drug for certain disease conditions (23). Similarly, Varghese et al. reported that transitions of care, use of over-the-counter and complementary medications may cause safety issues (24).
According to the results, a significant number of the nurses reported medical error, increased risk of drug-drug interactions, and adverse drug reactions as effects of PP and IMU. All these factors predispose the patients to the risk of cognitive impairment as well as disease progression. This finding is in agreement with the result of a previous study that reported an exponential increase in drug interaction following multiple medication use (25). Another study also revealed that taking unperscribed medications increases the risk of adverse outcomes (26). In fact, the inappropriate use of drugs may harm patients by reducing the quality of life and general well-being (27). Educating patients at discharge increases the chances of reducing repetitive therapy, inappropriate prescription, and intake of irrelevant medications (26).
Strength and limitations
Contrary to most studies with a focus on patient's knowledge of PP, especially among the older population, the present study assessed nurses' knowledge and perception of PP and IMU. We believe that our results can help promote effective PP management strategies that can assist policymakers initiate new programs or improve on existing ones. However, the study also had some limitations. First, the present study was conducted in a Nigerian State-owned teaching hospital. The utilization of a single research setting might limit the generalizability of the results as cultural variations across different States might influence nurses' knowledge of PP. Conducting studies involving more hospitals might give a truer picture of nurses' knowledge of PP and IMU. Besides, this study was limited by the small sample size (n=190), which might have impacted clinically important differences in the knowledge of nurses regarding PP and IMU effect.
Conclusion
The results indicate that the nurses working at the study setting possess good knowledge of PP and IMU. Furthermore, appropriate prescription, optimization of medications, health education, and periodic review of patients' medication were reported as means of preventing IMU. According to the subjects, medical error, risk of drug-drug interactions, adverse drug reactions, risks for cognitive impairment, and increased disease progression are some of the most important effects of PP and IMU. Based on the findings we recommend healthcare policymakers to initiate appropriate measures that will encourage more rational use of medications by patients and health care providers. Moreover, healthcare professionals should collaboratively work towards raising the level of awareness and knowledge about the effects of PP and IMU in order to reduce potential drug-related problems.
Indeed, PP is a problem of substantial importance in terms of both direct and indirect medication costs. Although nurses are less involved with the duty of drug prescription, however, nurses need to possess the ability to convince patients on avoidance of self-medication. Thorough educative advice will serve to reduce the stress imposed on nurses in managing the negative consequences of inappropriate drug use. Also, continuing education programs organized through routine professional training can translate nurses' knowledge into practice.
Acknowledgements
The authors would like to extend their sincere gratitude to the nurses who participated in this study.
Funding source
The study was self-sponsored by the researchers.
Ethical statement
The study was approved by the ethics and research committee of LAUTECH Teaching Hospital (Code: LTH/EC/2020/11/482). The principles of Helsinki declaration were upheld to protect the rights of individual participant recruited for the study.
Conflict of interest
Nurses are strategically positioned to ensure holistic healthcare services are provided to patients, especially concerning medication administration. In this regard, we assessed the knowledge and perception of nurses about the effects of PP and IMU on patients.
The knowledge level among our respondents was similar to findings of a cross-sectional study conducted in four tertiary care facilities in Nigeria. The study showed that the overall knowledge score was above average as most subjects (84.7%) were confident of their ability to prescribe rationally for elderly patients and to deal perfectly with clinical conditions affecting the cardiovascular, endocrine, and gastrointestinal systems (20).
The results of our study showed that 84.2% had good knowledge of PP and IMU, as 90% of the respondents have heard of PP and 87.4% agreed that PP is the use of different drugs for the treatment of a single disease. The high level of knowledge of nurses in our study can be related to their functional role and proximity to the patients in medication management. The knowledge possessed by nurses allows them to link the patient's symptoms to effects or side effects of the drugs prescribed (21) and to increase therapeutic effects of the prescribed medications.
In our study, 93.2% of the subjects agreed that IMU should be entirely avoided, and 64.2% claimed that PP can lead to IMU. This present study is at variance with the submission of a study that identified numerous reasons for Nurses’ lack of confidence in addressing PP as, considerations for withdrawal, inability to observe, stop or modify a previously prescribed drug, and other detrimental effects (13). Training programs that encourage continuing education of nurses and organization of seminars and workshops for care providers involved in medication management will reduce medication-related adverse outcomes (22).
Based on the results, having many co-existing conditions and chronic diseases is one of the reasons for PP among patients. Moreover, visiting multiple physicians for the same medical problem is another reason for IMU. Our subjects also stated that advancing age may predispose patients to IMU, which is in line with findings of a previous study (23). This could be due to the fact that chronic diseases are often more common among the older population. Patients suffering from comorbidities always require multiple medications to control symptoms. Also, increased availability of different medications might be another major factor that contribute to PP and IMU. This factor may have resulted in modification in the pattern of prescription, with the advent of a new specific drug for certain disease conditions (23). Similarly, Varghese et al. reported that transitions of care, use of over-the-counter and complementary medications may cause safety issues (24).
According to the results, a significant number of the nurses reported medical error, increased risk of drug-drug interactions, and adverse drug reactions as effects of PP and IMU. All these factors predispose the patients to the risk of cognitive impairment as well as disease progression. This finding is in agreement with the result of a previous study that reported an exponential increase in drug interaction following multiple medication use (25). Another study also revealed that taking unperscribed medications increases the risk of adverse outcomes (26). In fact, the inappropriate use of drugs may harm patients by reducing the quality of life and general well-being (27). Educating patients at discharge increases the chances of reducing repetitive therapy, inappropriate prescription, and intake of irrelevant medications (26).
Strength and limitations
Contrary to most studies with a focus on patient's knowledge of PP, especially among the older population, the present study assessed nurses' knowledge and perception of PP and IMU. We believe that our results can help promote effective PP management strategies that can assist policymakers initiate new programs or improve on existing ones. However, the study also had some limitations. First, the present study was conducted in a Nigerian State-owned teaching hospital. The utilization of a single research setting might limit the generalizability of the results as cultural variations across different States might influence nurses' knowledge of PP. Conducting studies involving more hospitals might give a truer picture of nurses' knowledge of PP and IMU. Besides, this study was limited by the small sample size (n=190), which might have impacted clinically important differences in the knowledge of nurses regarding PP and IMU effect.
Conclusion
The results indicate that the nurses working at the study setting possess good knowledge of PP and IMU. Furthermore, appropriate prescription, optimization of medications, health education, and periodic review of patients' medication were reported as means of preventing IMU. According to the subjects, medical error, risk of drug-drug interactions, adverse drug reactions, risks for cognitive impairment, and increased disease progression are some of the most important effects of PP and IMU. Based on the findings we recommend healthcare policymakers to initiate appropriate measures that will encourage more rational use of medications by patients and health care providers. Moreover, healthcare professionals should collaboratively work towards raising the level of awareness and knowledge about the effects of PP and IMU in order to reduce potential drug-related problems.
Indeed, PP is a problem of substantial importance in terms of both direct and indirect medication costs. Although nurses are less involved with the duty of drug prescription, however, nurses need to possess the ability to convince patients on avoidance of self-medication. Thorough educative advice will serve to reduce the stress imposed on nurses in managing the negative consequences of inappropriate drug use. Also, continuing education programs organized through routine professional training can translate nurses' knowledge into practice.
Acknowledgements
The authors would like to extend their sincere gratitude to the nurses who participated in this study.
Funding source
The study was self-sponsored by the researchers.
Ethical statement
The study was approved by the ethics and research committee of LAUTECH Teaching Hospital (Code: LTH/EC/2020/11/482). The principles of Helsinki declaration were upheld to protect the rights of individual participant recruited for the study.
Conflict of interest
The authors declare that there is no conflict of interest regarding publication of this article
Author contributions
Study conception and design: OOA, BDO
Data collection: OOA, BDO
Data analysis and interpretation: OOA, OA
Drafting of the article: All Authors
Critical revision of the article: OEA, OA, ZOO, KIJ, SOA
Data collection: OOA, BDO
Data analysis and interpretation: OOA, OA
Drafting of the article: All Authors
Critical revision of the article: OEA, OA, ZOO, KIJ, SOA
Type of study: Original Article |
Subject:
Nursing
References
1. World Health Organization. Medication safety in polypharmacy. Geneva: World Health Organization, 2019.
2. Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatrics. 2017; 17(1):1-0. [View at paplisher] [DOI] [PMID] [Google Scholar]
3. Khan N, Chattopadhyay K, Leonardi-Bee J. Incidence, prevalence, risk factors and health consequences of polypharmacy in adults in South Asia: a systematic review protocol. JBI Evidence Synthesis. 2019; 17(11):2370-7. [View at paplisher] [DOI] [PMID] [Google Scholar]
4. Khezrian M, McNeil CJ, Murray AD, Myint PK. An overview of prevalence, determinants and health outcomes of polypharmacy. Therapeutic Advances in Drug Safety. 2020 [View at paplisher] [DOI] [PMID] [Google Scholar]
5. Quinn KJ, Shah NH. A dataset quantifying polypharmacy in the United States. Scientific Data. 2017; 4(1):1-11. [View at paplisher] [DOI] [PMID] [Google Scholar]
6. Akande-Sholabi W, Adebusoye L, Olowookere O. Polypharmacy and factors associated with their prevalence among older patients attending a geriatric centre in South-West Nigeria. West African Journal of Pharmacy. 2018; 29(1):35- 45. [View at paplisher] [DOI] [Google Scholar]
7. Gbeasor-Komlanvi FA, Zida-Compaore WI, Dare IH, Diallo A, Darre TP, Potchoo Y, et al. Medication Consumption Patterns and Polypharmacy among Community-Dwelling Elderly in Lomé (Togo) in 2017. Current Gerontology and Geriatrics Research.2020. [View at paplisher] [DOI] [PMID] [Google Scholar]
8. Ssonko M, Stanaway F, Mayanja HK, Namuleme T, Cumming R, Kyalimpa JL, et al. Polypharmacy among HIV positive older adults on anti-retroviral therapy attending an urban clinic in Uganda. BMC Geriatrics. 2018; 18(1):1-8. [View at paplisher] [DOI] [PMID] [Google Scholar]
9. Lavan AH, Gallagher P. Predicting risk of adverse drug reactions in older adults. Ther Adv Drug Saf. 2016; 7(1):11-22. [View at paplisher] [DOI] [PMID] [Google Scholar]
10. Leelakanok N, Holcombe AL, Lund BC, Gu X, Schweizer ML. Association between polypharmacy and death: a systematic review and meta-analysis. Journal of the American Pharmacists Association. 2017; 57(6):729-38. [View at paplisher] [DOI] [PMID] [Google Scholar]
11. Sun W, Lam A. Raising awareness about the critical importance of the nursing role in deprescribing medication for older adults. Perspectives. 2019; 40(4):17-22. [View at paplisher] [Google Scholar]
12. Djerbib A. A qualitative systematic review of the factors that influence prescribing decisions by nurse independent prescribers in primary care. Primary Health Care. 2018; 28(3):25. [View at paplisher] [DOI] [Google Scholar]
13. Farrell B, Richardson L, Raman-Wilms L, de Launay D, Alsabbagh MW, Conklin J. Self-efficacy for deprescribing: a survey for health care professionals using evidence-based deprescribing guidelines. Research in Social and Administrative Pharmacy. 2018; 14(1):18-25. [View at paplisher] [DOI] [PMID] [Google Scholar]
14. Mecca MC, Thomas JM, Niehoff KM, Hyson A, Jeffery SM, Sellinger J, et al. Assessing an interprofessional polypharmacy and deprescribing educational intervention for primary care post-graduate trainees: a quantitative and qualitative evaluation. Journal of General Internal Medicine. 2019; 34(7):1220-7. [View at paplisher] [DOI] [PMID] [Google Scholar]
15. Campins L, Serra-Prat M, Gózalo I, López D, Palomera E, Agustí C, et al. Randomized controlled trial of an intervention to improve drug appropriateness in community-dwelling polymedicated elderly people. Family Practice. 2017; 34(1):36-42. [View at paplisher] [DOI] [PMID] [Google Scholar]
16. Sun W, Tahsin F, Abbass Dick J, Barakat C, Turner J, Wilson D, et al. Educating Homecare Nurses about Deprescribing of Medications to Manage Polypharmacy for Older Adults. Western Journal of Nursing Research. 2021. [View at paplisher] [DOI] [PMID] [Google Scholar]
17. Wastesson JW, Morin L, Tan EC, Johnell K. An update on the clinical consequences of polypharmacy in older adults: a narrative review. Expert Opinion on Drug Safety. 2018; 17(12):1185-96. [View at paplisher] [DOI] [PMID] [Google Scholar]
18. Engel RJ, Schutt RK. The practice of research in social work. Sage Publications; 2016.
19. Brown JD. The Cronbach alpha reliability estimate. Jalt Testing & Evaluation Sig Newsletter. 2002; 6(1). [View at paplisher] [Google Scholar]
20. Fadare JO, Obimakinde AM, Enwere OO, Desalu OO, Ibidapo RO. Physician's Knowledge of Appropriate Prescribing for the Elderly-A Survey Among Family and Internal Medicine Physicians in Nigeria. Frontiers in Pharmacology. 2019; 10:592. [View at paplisher] [DOI] [PMID] [Google Scholar]
21. Bell HT, Granas A, Enmarker I, Omli R, Steinsbekk A. Nurses' and pharmacists' learning experiences from participating in interprofessional medication reviews for elderly in primary health care-a qualitative study. BMC Family Practice. 2017; 18(1):1-9. [View at paplisher] [DOI] [PMID] [Google Scholar]
22. Huisman BA, Geijteman EC, Dees MK, Schonewille NN, Wieles M, van Zuylen L, et al. Role of nurses in medication management at the end of life: a qualitative interview study. BMC Palliative Care. 2020; 19:1-11. [View at paplisher] [DOI] [PMID] [Google Scholar]
23. Badawy NA, Labeeb SA, Alsamdan MF, Alazemi BF. Prevalence and Risk of Polypharmacy among Community-Dwelling, Elderly Kuwaiti Patients. Medical Principles and Practice. 2020; 29(2):166-73. [View at paplisher] [DOI] [PMID] [Google Scholar]
24. Varghese D, Ishida C, Haseer Koya H. Polypharmacy. [Updated 2021 Jul 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532953/
25. Johnell K, Klarin I. The relationship between number of drugs and potential drug-drug interactions in the elderly. Drug Safety. 2007; 30(10):911-8. [View at paplisher] [DOI] [PMID] [Google Scholar]
26. Valenza PL, McGinley TC, Feldman J, Patel P, Cornejo K, Liang N, Anmolsingh R, McNaughton N. Dangers of polypharmacy. InVignettes in Patient Safety-Volume 1 2017 Sep 13. IntechOpen. [View at paplisher] [DOI]
27. Schenker Y, Park SY, Jeong K, Pruskowski J, Kavalieratos D, Resick J, et al. Associations between polypharmacy, symptom burden, and quality of life in patients with advanced, life-limiting illness. Journal of General Internal Medicine. 2019; 34(4):559-66. [View at paplisher] [DOI] [PMID] [Google Scholar]
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |



